Reflections
My formative years between the ages of five and twenty-two were spent in the suburb of Woodville. As young kids during World War II, around the age of ten or so, we’d cycle along Woodville Road on our way to the salt flats that are now West Lakes, and then on to Grange Beach and the Henley Baths for a Saturday afternoon swim and a ‘bush biscuit’.
As we passed the Connor property, the house hidden behind dense shrubbery, we used to cycle that much faster, as rumour had it that the house was haunted and inhabited by strange people – small people – and we were in some danger if we got too close.
What an unforseen coincidence it was that, twenty years later, I should return to the Connor property, and spend my working life where the ‘haunted house’ once stood.
Re-reading this text I feel I may have dealt a little harshly with some of my colleagues. It behoves me therefore to give myself an assessment card after a lifetime of surgery.
Where would I put myself?
Probably in the middle range. A journeyman surgeon who was sound enough but did not reach the dizzy heights of many of those standout surgeons with whom I came in contact over the years.
Reflecting on the deaths of my patients over the years is salutary and worthwhile, so I shall do so.
I remember them all well. In the early days of TQEH, Dick Jepson initiated a Deaths Review Meeting held once a month and it was attended by all specialties. It was conducted under the auspices of the Pathology Department who decided which deaths passing through their portals could be considered controversial.
The initial sentiments of attendees – ‘there but for the grace of God go I’ – degenerated eventually into something of a witchhunt, leaving egos bruised and feelings hurt and so, after several years of very useful and instructive contributions, the meetings were abandoned.
At age 90 (and with three daughters!), my ego is used to being bruised and so I have no embarrassment in revisiting my mistakes.
I am still troubled to this day by the ghost of a Maori patient whom I attended in New Zealand back in 1958. His name was Keriopa Paki and he had torn a hole in his oesophagus swallowing a chop bone. I was on casualty duty as the sole medical officer shortly after I arrived as a raw recruit in New Zealand. The hospital had no ENT service and so I consulted the specialist anaesthrtist in theatre as we were about to start an 8.00 am operating list. He was not terribly interested but had a cursory look with his laryngoscope and found nothing so we discharged him. He returned a couple of days later with a roaring mediastinitis and demised after a few days. I was left to carry the can at the subsequent coroner’s inquest. The coroner was very kind to me and laid the blame entirely on this poor Maori for his stupidity in swallowing a chop bone! I felt I had been thrown under a bus by my seniors on that occasion, although I could have been more pro-active. No-one in the Wanganui Hospital put up their hand to help the raw novice and I was left to front the inquest alone.
The next was a ruptured middle meningeal artery at Croydon Casualty in England in 1963. This episode has been alluded to earlier. The patient arrived by ambulance and was drunk and incoherent when he arrived in the Casualty Department and had to be restrained. I was given no history of injury or fall by the ambulance officers, but nevertheless, I should have checked his pupils and may have found one non-reactive or fixed and dilated and should have immediately sent him to the famous Atkinson Morley Neurosurgical Hospital, down the road at Wimbledon, where the first CT scan was performed in 1971. A fail for the surgeon.
I had another death in the Croydon Casualty Department – a stabbing murder with the victim moribund on arrival in casualty. This resulted in a trip to the famous Central Criminal Court – the Old Bailey – near St Barts Hospital where I subsequently attended a course for the FRCS. After giving evidence, the lawyer for the prosecution took me for a pint at the adjacent, famous Magpie and Stump Hotel, from the upper floors of which it had been possible in the 18th century to watch the hangings at the infamous Newgate Prison which stood opposite the hotel.
The next was early in my career back in South Australia – a 60-year-old woman with a leaking diverticulitis of the sigmoid colon. At operation in TQEH, we discovered an infected fixed mass that was irremovable and so it was drained. Thereafter, she failed to settle, with recurrent flare-ups necessitating redraining over subsequent weeks. Eventually, she died. I don’t believe I performed a defunctioning colostomy, which may or may not have saved the day. Another fail.
Trauma to the liver in those early days was always a problem. I remember at least one patient dying on the table in the middle of the night following a car accident. There were no specialist liver surgeons in those days.
One liver rupture does stick in my mind. The main approach to a damaged liver was to pack it and resuscitate the patient, to try to get control of the situation. On the night in question, we called in two anaesthetists and, with repeated packing and rapid transfusions, we gradually gained the upper hand. I opted to leave four or five large packs in the wound and the patient was sent to intensive care. I was due to leave the country a couple of days later, so I asked my good friend Trevor Pickering to put the man on his Friday operating list and remove the packs. Trevor obliged and, when I returned a couple of weeks later, the patient was about to be discharged.
The next patient was a Jehovah’s Witness with a large cancer of the rectum. He and his family realised the risks of not accepting blood in such a procedure and were adamant they would not allow any blood to be transfused. We had moderate haemorrhage during the operation which would have been easily controlled with a couple of units of blood. However, it gradually became apparent that we were falling behind. I de-gloved and went out to persuade the relatives to allow us to transfuse. They were adamant that no blood was to be given: “We accept God’s will”, they told me.
Towards the end of the procedure, it became apparent that the patient was bleeding almost pure plasma and substitutes, with no oxygen-carrying capacity. It was very upsetting and I believe he died unnecessarily. I resolved thereafter to disobey their teaching if ever the situation arose again and let them have their day in court.[1]
The final case I recall was a private patient admitted as an emergency to TQEH with a small bowel obstruction. A segment of the bowel was gangrenous but I had no reason not to think a good result was not achievable with resection and anastomosis.
I was in the habit of getting a private anaesthetist in to the public hospital for private cases rather than using staff anaesthetists and, on this occasion, the anaesthetist my office had arranged did not have a higher degree and, as it turned out, was not skilled or experienced enough to manage. Halfway through the operation, things started to go pear-shaped and I noticed the blood was blue and not pink. We called for senior hospital anaesthetists and they attempted to retrieve the situation but, alas – too late; the patient died. It remains the surgeon’s responsibility to select an anaesthetist fit for the task in hand. Another fail.
In the early days, general surgeons were just that: general surgeons who did everything, or almost everything. I had good training in urology both in England and under Noel Bonnin at TQEH. I continued to do prostatectomies long after it became the province of urologists and considered excluding that procedure from my repertoire when trans-urethral procedures became the norm. One of the last I did was at Calvary and the retropubic procedure went satisfactorily, I thought.
From the operating theatre I had gone to the District Court to give evidence in a Workers’ Compensation case. I was in the dock giving my evidence when suddenly my beeper went off. It was before the days of mobile phones and we were contacted by our secretaries by a beeper which sounded rather loudly. The Magistrate intervened and politely asked, “Doctor would you like us to suspend the Court while you attend to your call?”
“Thank you, your Honour, I would be most grateful,”I replied.
The message from Calvary was that the prostatectomy I had done earlier was bleeding from the catheter a little more than they would like. The theatre charge nurse, Sister Liz Mazey, was on the other end of the line. She was an excellent nurse with whom I am still in contact.
What to do? Tell the magistrate I would have to go and for him to reconvene the court? Take a chance on the bleeding stopping?
Sister Mazey, bless her, provided a solution. John Jose, a urologist was doing a list at the time and she knew he would be happy to help out. I agreed.
I returned to the court. “Everything alright?” asked the Magistrate.
“Yes Sir,” I replied, and resumed my evidence.
I was not at all unhappy to call time on the active practice of surgery at the end of 1998 and looked forward to the other interests I had in mind. As earlier mentioned, I did continue my medico-legal practice for two to three days a week for about three years and enjoyed the work, particularly the jousting in the court room where I found even the Senior Councils quite ignorant on medical and surgical matters. None of them had any training whatsoever in this direction.
When I did retire from operating at the end of 1998, Professor Guy Maddern approached me and said he had just the retirement job for me. It would involve peripatetic surgery – spending a week or two doing emergency operating in various hospitals around South Australia – Mount Gambier, Whyalla, Port Lincoln, and so forth. I declined with thanks. Surgery is a high risk business, even higher risk in country towns, and I looked forward to retiring to a life not involving high risk, or at least limited to risks of my own choice.
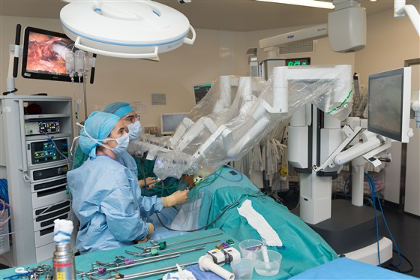
The Da Vinci Robot in action
One final experience I did enjoy later in my retirement was attending a world hernia conference in Adelaide at the invitation of my good friend, Alex Karatassas, in 2019. In the trade display area, they had set up a Da Vinci robot with a mock patient. In a quiet period, I managed to persuade the attendant to give me a lesson at the controls. I was entranced by the superb vision one was afforded whilst sitting at the hand controls and the ease with which the instruments could be guided to their target from such a remote position. What a brave new world surgery has entered!
How lucky I have been!
Lucky to have been involved in a profession which I have loved and looked forward to being involved in every day. A feeling of reward was experienced at the end of each day, not necessarily from the thanks expressed by patients, but by the knowledge that each day was spent in a worthwhile cause. Lucky to have had such good work companions.
Most of all lucky to have a wife and family who were prepared to make the not inconsiderable sacrifices necessary to allow me to indulge myself in a passion.
[1] Jehovah’s Witnesses interpret the following Biblical passage addressed to the gentile Christians as a direction to avoid blood transfusions: Acts 15; 28-9.
For it has seemed good to the Holy Spirit and to us (the apostles and elders) to lay on you no greater burden than these requirements: that you abstain from what has been sacrificed to idols, and from blood, and from what has been strangled, and from sexual immorality.
You do look, my son, in a moved sort, As if you were dismay’d. Be cheerful, sir. Our revels now are ended. These our actors, As I foretold you, were all spirits and Are melted into air, into thin air: And, like the baseless fabric of this vision, The cloud-capp’d towers, the gorgeous palaces, The solemn temples, the great globe itself, Yea, all which it inherit, shall dissolve, And, like this insubstantial pageant faded, Leave not a rack behind. We are such stuff As dreams are made on, and our little life Is rounded with a sleep.[2]
[2] Shakespeare, The Tempest (Prospero)as quoted in Helgoland by Carlo Revelli, Penguin Random House UK,
.
