Sussex and home
After we packed and said our farewells at Epsom, we travelled in our recently replaced vehicle, an ancient Bedford Dormobile, loaded with all our gear, including baby Anne, to Southlands Hospital, Shoreham-by-Sea, Sussex.
On arrival, we found that our promised attractive flat at the back of the hospital had been given to a house surgeon. Not at all pleased with this development, I objected strongly to the authorities and declined to unload to the lesser site which they had offered. A third site was found, this time the Matron’s bungalow, just inside the main hospital entrance. It was charming, with three bedrooms, a lovely sitting room with a fireplace and opening through French doors to a glorious lawn and garden. There was a second well-furnished sitting room. It was fully enclosed by hedges from the hospital making it completely private. A lovely conclusion to our English accommodation and by far the most comfortable. The hospital gardeners maintained the garden and cut the lawns.

The Matron’s bungalow was great accomodation for our last year in England
1965 was certainly our most enjoyable both for me professionally and, I think, for Sadie, as the accommodation was ample and we developed a happy social life.
My job was initially predominantly orthopaedics, which I enjoyed as I had a pleasant and up-to-date boss, a New Zealander, John Addison. He had me doing the latest you-beaut procedure in no time – the Austin Moore prosthesis – for fractured necks of femurs.
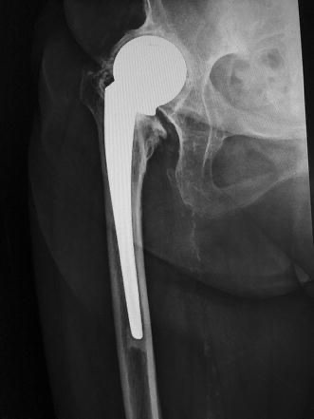
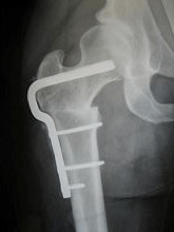
McMurray osteotomy L and Austin Moore prosthesis R
John had developed his own technique for this and had his anaesthetist photograph the whole procedure on super-8 film so he could show it at orthopaedic meetings. The Charnley hip procedure was just coming into vogue and he was about to swing over but in the meantime he had me doing a McMurray osteotomy for osteoarthritis of the hip, a procedure which did not have a very long shelf life. It was designed to alter the weight-bearing of an OA hip and thereby relieve pain.
The south coast of England was the retirement haven for the aged and wealthy, and so we had a plethora of fractured hips and prostatic obstruction. Clinical material for me was plentiful and with the NHS they were nearly all public patients and so it was worth the consultants while to train me up so I could help them carry the load.
I learned all the orthopaedic operations – arthrodeses, amputations below knee and above knee, de Quervains, fractures of all varieties, K-nails for femoral fractures, Kellers for bunions, menisectomies, Baker’s cysts, Zadeks, plating of forearm fractures, pins for humerus fractures, patellectomies and ruptured Achilles tendons. Addison also showed me how to do a laminectomy for spinal disc prolapse and I did one or two but felt this was really a neurosurgical procedure, having done six months neurosurgery in Australia, so I bowed out of any more. Certainly I would not be including disc surgery in my repertoire as an orthopaedic surgeon, although it was commonly included in general orthopaedic practice at the time.
The policy on the unit for the numerous fractured hips we saw was to go directly to a replacement prosthesis for a subcapital fracture, rather than a Smith Peterson pin, which more often than not resulted in necrosis of the head of the femur, necessitating a second operation in a frail patient. I probably did 25 to 30 Austin Moores and that stood me in good stead at The Queen Elizabeth Hospital as a senior registrar later.
My predecessor in this job had been Tom Stevenson. He had moved on to have a registrar job in orthopaedics down the road at Brighton General Hospital but had developed a close rapport with John Addison and continued to turn up to our weekly Friday orthopaedic lists to check up on his former boss. I did not know Tom very well in those days but silently objected to him turning up for our Friday list, as I felt I deserved first bite on all the clinical material.
Sadie became friends with Tom’s wife Cathy and we were very surprised when they migrated to Adelaide, after which they numbered amongst our closest and dearest friends. Tom became one of Adelaide’s most respected and skilful orthopaedic surgeons and deservedly had an operating theatre at The Queen Elizabeth Hospital named in his honour. Tom was totally dedicated to his profession and had a reputation for turning out at any time of the day or night, weekends included, if someone rang with a problem, whether or not it was one of his referring GPs.
‘Huffey’ McLean was the other new Zealander at Southlands Hospital. He was a charming, older man with a marked limp. Certainly he was up to date with breast cancer trends and had me doing preservative Patey mastectomies in preference to the traditional radical mastectomy, a mutilating procedure.
I remember the first Patey I did at Shoreham. We were in the habit of doubling up with our operating lists, utilising the anaesthetic room as another operating theatre in order to get through more cases from our bulging operating lists. On this occasion, Huffey was doing a major case in the operating theatre and I was doing a frozen section on a breast in the anaesthetic room. Unexpectedly, the frozen section came back positive and Huffey from the main theatre told me to get on and do a Patey mastectomy. I had not previously done that operation and normally was in the habit of going over any new procedure carefully the night before. However, I had a good idea as a Patey was much easier than a radical mastectomy and it all went off well.
Huffey was a genuine, nice man. Upon the birth of our second daughter in Southlands Hospital, he presented us with a pheasant and a bottle of French Beaujolais.
The doubling up was also a regular event on the orthopaedic side – the two NZ surgeons made a habit of it! On the Friday afternoon orthopaedic list there were two operating tables squeezed into one theatre and one anaesthetist, a Dr Burton, gave the two anaesthetics synchronously side by side, with an anaesthetic nurse squeezing one bag under Burton’s watchful eye as he simultaneously administered the second anaesthetic.
John Addison, the orthopaedic surgeon, was at the time preparing an 8mm film to present at the Royal Society on his experiences with Austin Moore prosthesis, so Burton was the camera man as well as double anaesthetist. It was fascinating. After the list on a Friday evening, Addison would be off to the pub and, after a couple of beers, he would get a twinge of conscience and ring me up at the hospital: ‘Johnson, did we take the tourniquet off that last Kellers patient we did?’ I was always able to reassure him so that he could settle into his next beer.
One other feature of the orthopaedic unit at Shoreham was their insistence on using a non-touch technique, the theory being that gloves are unreliable and cannot be guaranteed against perforation, particularly if forcible use of the hands is necessary. Other aspects included all needles being threaded with the help of two pairs of forceps, ligatures touched only with forceps and scissors and tied with forceps. No hands go anywhere near the patient’s wound. After a little practice, the technique becomes second nature.
I found this technique was not in vogue on returning to Adelaide, even in orthopaedic circles. As orthopaedics was to become a lesser part of my practice I did not continue with it.
The third surgeon for whom I worked at Shoreham was K. Whittle Martin, a talented Urologist who had undoubtedly been drawn to the south coast where there were plenty of wealthy, ageing males who required private attention for their enlarging prostates. Of course, there was the inevitable overload of NHS patients, so he gave me a Friday morning list to myself filled purely with the non-paying prostatectomies. The theatre he gave me for this list was a funny little room away from the main theatres, with a visitors’ corridor directly outside. It was not unusual for the door to be opened by a visitor in the midst of me doing a prostatectomy. ‘Where do we go to catch the Worthing bus?’ I remember was a popular request from these visitors with one foot inside our sterile operating theatre. ‘First corridor on your left, follow it to the next door and then you’ll see the sign,’ they were told by my anaesthetist who failed to blink an eyelid. ‘Thanks very much,’ would be the reply as they closed the theatre door.
K. Whittle Martin was knowledgeable, technically competent, suave and a good teacher but I felt he took advantage of underlings. He had a private practice at Littlehampton, half an hour down the coast, where he consulted and operated on his private patients. He asked me to assist at his operations on my afternoons off, to which I always agreed. At other times, he would ask me to do his private consulting at Littlehampton, when he had better arrangements. To this also I agreed. It was above and beyond my hospital contract and so I expected appropriate remuneration. I kept a record and when no remuneration was forthcoming and I had booked our passage home I approached him and presented my account – a considerable bill. I had expected a confrontation but he was all apologetic, saying it was an oversight and promptly settled my account on the spot. I guess he took the attitude that you win some and you lose some with transient registrars. Maybe those staying in England cannot afford to upset their seniors.
My predecessor in this job had been one Michael Hamilton who went on to become a well-recognised urologist back in Adelaide at the RAH, his father ‘Shorty’ having been one of my Surgical Honoraries as a student.
The fourth surgeon to whom I rotated was probably the most amazing and talented surgeon that I ever encountered in almost 40 years of surgery. His name was Charles Heanley.
Heanley was born in Hong Kong and educated at Epsom College and then at Downing College, Cambridge. With the inception of the National Health Service by its architect Aneurin Bevan and the Labour Government in July 1948, Charles Heanley was appointed as consultant general surgeon to the Worthing Group of hospitals. He had already been appointed surgeon in charge of the Department of Plastic Surgery at the London Hospital, having returned there after service in Dan Camiers, France and later at Ranikhet, 6,000 feet up in the Himalayas in India. At Ranikhet, during 1941 and 1942, where he had been sent after training with the renowned father of plastic surgery, Sir Harold Gilles, he had been commanding officer of number three British Maxillofacial Surgery Unit with the rank of Lieutenant Colonel. ‘We worked in the theatre from 9 until 6pm, three days a week, recovering on alternate days and hoping our patients would do the same!’ he said.

Heanley was a consultant at the Queen Victoria Hospital, East Grinstead (above) where disfigured WWII soldiers and airmen were transferred. The facility is recognised as the birthplace of modern plastic and reconstructive surgery under the auspice of Archie McIndoe. Patients referred to themselves as ‘The Guinea Pig Club’ ‘
In addition to his appointments at the Worthing Group and the London Hospital, he had an appointment, amazingly, as consultant ENT surgeon at the Luton and Dunstable Hospital in Bedfordshire, north of London.
Certainly, Heanley’s ENT prowess was confirmed to me in later years by an Adelaide ENT surgeon at the Queen Elizabeth Hospital, Ken Jones, who had received his training in ENT at the London Hospital from Charles Heanley. He, too, was in awe of the man’s surgical prowess.
Neville Minnis, ENT consultant surgeon at TQEH, also came in contact with Heanley at The Royal National ENT Hospital at Gray’s Inn Rd, London, where Heanley had an another appointment.
One thing which struck me about Charles Heanley was that he thrived on living on the edge. He had a sleek, powerful Jaguar which he drove exceedingly fast. It was recorded that he had been pursued by a police car down the A24 from London to Worthing and they caught up with him as he sprinted from the Worthing Hospital car park to start his (supposed) afternoon operating list. Whether he received a driving conviction or talked his way out of it is not known. Certainly he must have spent many hours driving his beloved Jag as Worthing was 95km south from London along the A24 and Luton was 53 km north along the M1 Motorway which would have made for easier driving.
One’s impression was that he considered himself to be on an higher strata than the other consultant surgeons on the south coast and consequently had few friends among his peers and certainly did not socialise with them. Two of the consultant surgeons at Southlands were New Zealanders and this may have contributed to his aloofness. For my part, as his registrar and his only contact in the hospital, I found him friendly and helpful, with no prejudice towards my antipodean origins.
On one occasion I had cause to ring him at about 2.00am. He answered the telephone in typical upper class fashion, ‘Hainley har.’
‘Oh, it’s Johnson Sir, we have a bleeding duodenal ulcer which I think needs operation.’
‘Well Johnson, get the theatre ready for twenty minutes and I’ll be over.’ He lived close by, somewhere in West Sussex.
One’s wish of course, as a training registrar, would be that the consultant would assist the trainee but understandably, in the middle of the night, this was rarely the case. It would be either, ‘You’ll manage that OK – ring me if you can’t’ or ‘I’ll do it’.
Heanley duly arrived in his Jag at Southlands Hospital and we all scrubbed up. The patient was anaesthetised on the table and the abdomen was cleaned and draped. At this stage, Heanley indicated to the scrub sister to move around to his side. Standard procedure was for the surgeon to operate with the assistant opposite on the other side of the patient and the scrub sister positioning herself on the assistant’s side together with her trolley of instruments but nearer the patient’s feet. With this normal setup, the surgeon would not need to turn to receive the required tool.
The request by Heanley on this occasion was curious but the sister obliged, whereupon Heanley positioned her trolley alongside his left elbow and told her to stand on the other side. It then became obvious what he had in mind. He would be his own scrub nurse and help himself to the tools as required – no asking and no receiving – much quicker. It was a joy to watch the complete master surgeon at work. No wasted movements, no hesitation. Gastrectomy completed in twenty minutes. Normally, the procedure would take two hours in the most skilled hands, three in the less skilled. He was back home in the cot inside an hour. And, yes, the patient recovered very well.
On another occasion on one of his regular lists we had a hair lip to repair in a baby. Again, Heanley dismissed the scrub nurse as being redundant. He arranged the baby and the drapes such that the baby’s head was cradled in his seated lap and the instrument trolley was alongside. The anaesthetist was not wildly excited by the arrangement but managed. Heanley was a surgeon par excellence.
To his credit he did teach me how to do ‘bat’ ears. He thought it would stand me in good stead ‘down under’. He showed me how to take an ellipse of skin and then an ellipse of underlying cartilage at the back of the ear and put it all together. I think he may even have allowed me to do the other side. So much for bat ears – not one ever crossed my threshold!
In correspondence to the British Medical Journal in 1970, several years after his retirement, he made the interesting observation that injection of vital blue dye into any part of the breast showed lymphatic drainage to both retrosternal glands and the axilla. He also noted that dye injected into the hand tracked randomly through the axilla and it was not possible to avoid lymphoedema of the arm by conserving particular lymphatics. He had an interest in lymphoedema.
Heanley retired in 1965 at the age of 58 which was, coincidently, the year I spent working for him at Shoreham. I trust I had no connection to that event. His recreations were swimming and archaeology. He had three sons, two of whom became doctors. He died just before his 101st birthday in February, 2008, and was buried at Hamsey Church, East Sussex, a parish church built well before the Norman Conquest in 1066.

Hamsey Churchyard, East Sussex
The history of Southlands Hospital is worthy of a paragraph. Following the passing of the Poor Law act in 1834 the parishes of East and West Sussex joined together to form the Steyning Union. The Union workhouse was built in Ham Road shortly after, all of this being in response to the massive unemployment in the years following the Napoleonic Wars.
Able-bodied men were no longer to receive relief in cash. Instead they were to go to one of those gaunt workhouses which were being built up and down the country. Life in the workhouse was to be made so unpleasant that nobody would apply for relief who was capable of earning an honest living. The standard of living in the workhouse was to be lower than the lowest that could possibly be expected outside. And in the squalor of early industrial England, that standard was unspeakably low.
Jonathan Sumption in Southlands Workhouse and Hospital, League of Frtends of Southlands Hospital, 1998, p.7
The architect and philosopher of the Poor Law was George Nicholls, who wrote:
I wish to see the poor-house looked to with dread by our labouring classes, and the reproach for being an inmate passed down from father to son. Let the poor see that their parish, although it will not allow them to perish through absolute want, is yet the hardest taskmaster, the closest paymaster, and the most harsh and unkind friend they can apply to.
Southlands Workhouse and Hospital p.7.
By the end of the 19th century, a much more humane regime had been instituted in most places, when it was recognised that many of the population were not poor because they were work shy but rather through personal incapacity, indifferent health, or mental problems. They include a large number who were aged and infirm and could no longer look after themselves.
And so over the years there was a gradual transition to a more caring establishment and finally in July, 1932, the workhouse, known as the Steyning Institution, was renamed Southlands Hospital.

Southlands Hospital around 1900
We had twelve happy months at Shoreham-by-Sea, and during nine of those months Sadie was pregnant with Catherine, our second born. During this pregnancy and during the European summer we rented a villa in Estartit, a tiny village on the Costa Brava in Spain, near Barcelona. A friend of mine from medical school days, Malcolm Symonds, had been appointed Professor of Obstetrics and Gynaecology at Nottingham University, and we arranged for him and his wife Sue and young children, Ian and David, to join us for the two-week holiday. Our trusty Bedford van was to be the transport for the four adults and three children, Anne being some eighteen months old at the time.
We travelled by ferry across the channel and commenced our trip down through the centre of France to the Spanish border. All went well until we reached Poitiers in Central France. The head winds and heavy load on board were too much for our ageing Dormobile and the clutch burnt out.
What to do? It was a Saturday afternoon and we managed to limp into the centre of the town. As luck would have it, there was a Bedford agent in Poitiers and when we located him he was just winding up for a restful weekend. Malcolm spoke reasonably fluent French and was able to indicate our predicament. To his credit, and recognising that in those days (1965) the French were not too kindly disposed towards Anglophiles, he kindly agreed to keep his garage open, climb down into his pit beneath our van, and replace the clutch, all on the Saturday afternoon. We were very impressed and took our families into the town to have some lunch.
When we returned a couple of hours later, he was still in the pit making rude noises about British products but eventually he finished the job, asked for a modest remuneration, and we were able to continue on our way.
Our route traversed the beautiful Loire valley so we spent a day or two exploring this centre of French culture with its magnificent chateaus and vineyards.
Crossing the border into Spain was a bit harrowing as in those days Spain was still under the dictatorship of Franco and the heavily armed soldiers at the border with France were a bit intimidating and suspicious of travellers. It was not until 1975 that Spain made the transition to a democracy.
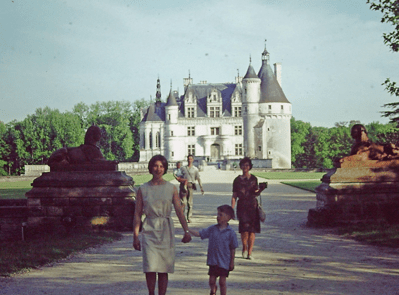
A stop-off at a chateau in the Loire Valley – Sadie and Ian ahead of Sue, David and Malcolm
Once we reached our villa in Estartit and settled in we were very comfortable. A maid was supplied with the villa and she did all the shopping and cleaning, cooked lunch and prepared the evening meal for us before she left.


Villa at Estartit, Costa Brava
Other notable activities at Shoreham included the annual trip up to Twickenham for the seven a side rugby tournament. As two of the consultant staff were new Zealanders this was a compulsory excursion.
The surgical section of the hospital was closed for the day and the surgical staff transported themselves en masse to Twickenham. We travelled with John Addison, if I remember correctly. Traditionally there was a stop at a pub halfway to London where everyone was well lubricated and then we moved on to the carpark at Twickenham. We could not help but notice the contrast between the rugby crowd gathering at Twickenham and a normal soccer crowd. These people were dressed in their tweed jackets and cloth caps and travelled in jaguars and other expensive cars. In the carpark, the boot was opened and we were each supplied with a pipkin of beer – equivalent to three litres – and this was meant to sustain us for the rest of the day.
It was a great occasion with all the London rugby clubs pitted against each other but restricted to seven players only in each side. After the final at about 4.00pm, we set off back to Shoreham, again with the compulsory stop at the halfway pub to bid each other farewell. I hasten to add that this was long before the days of blood alcohol testing.
As it had been at Epsom, so too it was at Shoreham. The highlight of these two years was the welcoming of a baby, Catherine Louise, born on November 11, 1965. She was our biggest and longest baby – again born with a thick thatch of hair.
The maternity ward was a happy place at Shoreham. The buxom Irish midwife was delivering the children of the babies she had delivered years before.

On one occasion, she was the only one on the ward when a patient went into labour, the labour ward being alongside the postnatal ward.
She knew Sadie was a trained midwife so she came rushing into her room;
‘Ach, Mrs Johnson, you’ll be giving the anaesthetic, won’t you!’
And before Sadie could reply, she was wielding the mask with gas and oxygen in the labour ward.
Baby Catherine, a few days old – another ‘Beatle’
On another occasion, one of the mothers had a birthday, so tables were set down the centre of the ward streamers and balloons were brought in together with a cake and everyone had a happy time.
On the day of Sadie and Catherine’s discharge, the old Irish sister said to Sadie, ‘Now mother, before the evening feed ye’ll be havin’ a large gin, and then you and the baby will be sleepin’ all night. And don’ be givin’ the baby milk, those cows in the Midlands eat grass covered in factory soot and it’s not healthy!’
What were our plans for 1966? Registrar jobs were only one-year appointments in the UK and by this time we were getting homesick and had decided to make our future in Adelaide. Trevor Pickering had returned to Adelaide and had written to me from The Queen Elizabeth Hospital where he had a three year appointment as a senior registrar. He wrote ecstatically of the atmosphere among the staff and the standard of surgery. He suggested that I should apply for a similar job for 1966.
Trevor’s letter acted as a stimulus and sometime in mid-1965 I sent a carefully-worded letter to Bob Magarey, one of three Senior Surgical Consultants at TQEH, indicating that he may not remember me but that I had been on his clinic and that I had been convenor of the Medical Students Dinner at the Myer Apollo dining room in 1957 when he was Chairman of the Medical Students’ Society, and that in that role he and I had worked fairly closely. I saved my coup de grace until last and noted that I was married to Sadie Marr, whom I knew had been one of his favourite sisters at the Memorial Hospital and on whom he had operated on for an ingrowing toenail in 1960.
This last revelation, I believe, carried the day, and before long I had an aerogramme from Bob telling me that indeed, he remembered both of us well, and offered to personally approach the Medical Superintendent, Doug Carmen, to write and offer me a Senior Surgical post commencing February 1, 1966. Surprisingly, he did not ask for any references, presumably accepting that FRCS England was enough.
Well, this was good news indeed, having employment for the next three years without having to front up for wretched interviews. The Queen Elizabeth Hospital had been opened by Queen Elizabeth herself in 1958 with the first patient admitted in 1959, so it was brand spanking new, without the old hierarchic structure of the Royal Adelaide Hospital. It was a teaching hospital with a research department, had young enthusiastic staff, top theatres and I would be involved in teaching medical students. My cup was full at that stage and it seemed our journey to UK had not been in vain, as I had certainly thought at one stage.
A word about Doug Carmen, who was on the Administration side of TQEH, employed full time by the Health Department. He worked in tandem with the lay hospital administrator Ken Treagus, to ensure the hospital functioned efficiently on a day to day basis. I became good friends with Doug, initially as a senior registrar and later on as a visiting staff consultant and finally as his treating surgeon. Doug had wanted to be a surgeon and initially embarked on a surgical career as a surgical registrar at the RAH under Sir Ivan Jose or Sir Phillip Messent. However his religion as a member of the Plymouth Brethren sect forbade him to join lay organisations including the Royal Australasian College of Surgeons. Doug even attained a Master of Surgery which is awarded by thesis. Because of his religion he abandoned his surgical ambitions and became Medical Superintendent at the Bedford Park Sanitorium for patients with pulmonary tuberculosis. At that time, just after WWII, patients with pulmonary tuberculosis were paid a pension – so long as they had a positive sputum or positive gastric washings. The patients from the Sanitorium would frequent the front bar of the nearby Flagstaff Hotel and buy and sell positive sputa thus enabling the buyer to keep his pension. The going price was five shillings a specimen. Doug’s house surgeon at the time relayed to me the story whereby a patient had absconded to the hotel and the said house surgeon had to take Doug to the Flagstaff front bar to retrieve the said patient. It would have been the only time in Doug’s life that that he set foot in such an institution.[1]

Doug’s religion forbade him to break bread with non-believers so he always dined alone in TQEH cafeteria. In addition he believed in street preaching so occasionally after his lunch he would go down Woodville Road and stand on his soapbox outside the Savings Bank and proclaim his beliefs.
Doug Carmen
Sometime after Doug retired, I had the privilege of being asked to repair his hernia. He insisted on being a public patient in a six bed bay. As I recall, he had no medical insurance and certainly declined the offer of a private room.
I could not help reflecting on bygone days, going back to World War II years in the 1940s, when as kids we used to peddle our bikes along Woodville Road, past the densely wooded acres belonging to the Connors. Members of the family living there at the time suffered from dwarfism and as ignorant children will, we scared each other with stories about them.
Come December, we said our farewells and travelled by train to Southampton, having sent our trunks ahead. There we boarded the Fairsea and the next day – a cold, miserable December day – we cast off on the five week voyage.




Farewell to England aboard the ‘Fairsea’ with Catherine just five weeks old
From memory, I think Sitmar Lines did not take babies less than two months old on board but somehow we managed to beat that restriction.
The voyage home was anything but a pleasure cruise and was, without doubt, the hardest of my three ship’s surgeon jobs.
When we embarked there was no heating on board as the Sitmar line was employed by the Australian Government to transport migrants as cheaply as possible to Australian shores.
As we sailed out from Southampton, the sea became very rough and on the second day I was forced to retire to my bunk with severe sea sickness. We had 800 adults and 500 children on board a ship designed to carry half that number. No sooner had I become horizontal than a nurse arrived informing me there were 25 patients waiting to see me. There were two other Italian doctors on board but they spoke no English so, in effect, I was the sole doctor. I told the nurse to go away but she soon returned with an injection of Stemetil and waited until I staggered out of my bunk and followed her to start seeing patients.
The children came from all corners of England and carried every strain of infection with which to cross infect each other. We had three epidemics of chicken pox during the trip and I was convinced that we were going to lose at least one poor little waif, an eight-year-old skinny child with pneumonia who spent the whole trip in our hospital – which remained mostly full with around 40 patients. This little girl miraculously survived the trip and I insisted that she leave the ship in Perth, with her parents, where good facilities were available.
Meanwhile, Sadie had her problems looking after our five-week-old as it was difficult to keep bottles sterilised. Anne lost a lot of weight as she had a persistent ear infection which was drained as soon as we arrived in Adelaide.
In the 1960s, voyages UK to Australia all passed through the Suez Canal in Egypt. It was customary for passengers to be given the option of disembarking in Port Said and travelling to Cairo to visit the pyramids and the Cairo Museum before returning to pick up the ship at Suez in the Red Sea after it had traversed the Suez Canal. This was a full day’s trip. I had been working flat out for some three weeks so decided to take my first day off for sight-seeing. It wasn’t at all fair on Sadie who had been working equally as hard looking after a baby and a two-year-old.
During that day, as the ship sailed through the Bitters Lake on route to Suez, the ship’s captain happened to bump into Sadie on deck and enquired as to my whereabouts. He was mightily displeased when he heard I had gone AWOL and upon my return let me know in no uncertain terms. As was my wont,I humbly accepted his reprimand.
How good it was to meet all our family in Adelaide after four long years and how pleased they were to meet two new members of our family.
Beginnings of TQEH in 1956 – ‘haunted house’ bulldozed!‘

[1] Bill Proudman’s book In the Beginning: the formative years of The Queen Elizabeth Hospital is a detailed history of the hospital’s contribution to medical innovation. Details here.
READ Chapter 11
